Abstract
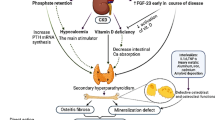
Chronic kidney disease (CKD) is complicated by disturbances of mineral and bone metabolism which start early in the course of the disease. It has long been assumed that high turnover bone lesions induced by secondary hyperparathyroidism are the predominant type of renal osteodystrophy from the start. However, there is increasing evidence in favor of the view that in early CKD stages low bone turnover is prevailing, with adynamic bone disease being the predominant form. Since serum parathyroid hormone levels increase progressively early on, and the most probable explanation is resistance to the skeletal action of this hormone. An early inhibition of the Wnt pathway with an increase in sclerostin and other inhibitors of Wnt signaling may be involved. Finally, a variety of other uremic toxins such as indoxyl sulfate and phosphate may play an important role in the pathogenesis of the low turnover bone disease observed in early stages of CKD. The optimal strategies to prevent and to treat adynamic bone disease in incipient CKD yet need to be defined. Targeting uremic toxins such as sclerostin, phosphate, and indoxyl sulfate may be relevant.


Similar content being viewed by others
References
Kidney Disease-Improving Global Outcomes (KDIGO) CKD-MBD Work Group (2009) KDIGO clinical practice guideline for the diagnosis, evaluation, prevention, and treatment of chronic kidney disease-mineral and bone disorder (CKD-MBD). Kidney Int Suppl:S1–S130
National Kidney Foundation (2003) K/DOQI clinical practice guidelines for bone metabolism and disease in chronic kidney disease. Am J Kidney Dis 42:S1–201
Barreto FC, Barreto DV, Moyses RM, Neves KR, Canziani ME, Draibe SA, Jorgetti V, Carvalho AB (2008) K/DOQI-recommended intact PTH levels do not prevent low-turnover bone disease in hemodialysis patients. Kidney Int 73:771–777
Malluche HH, Mawad HW, Monier-Faugere MC (2011) Renal osteodystrophy in the first decade of the new millennium: analysis of 630 bone biopsies in black and white patients. J Bone Miner Res 26:1368–1376
Sprague SM, Bellorin-Font E, Jorgetti V, Carvalho AB, Malluche HH, Ferreira A, D’Haese PC, Drueke TB, Du H, Manley T et al (2016) Diagnostic accuracy of bone turnover markers and bone histology in patients with CKD treated by dialysis. Am J Kidney Dis 67:559–566
Sherrard DJ, Hercz G, Pei Y, Maloney NA, Greenwood C, Manuel A, Saiphoo C, Fenton SS, Segre GV (1993) The spectrum of bone disease in end-stage renal failure—an evolving disorder. Kidney Int 43:436–442
Coen G, Mazzaferro S, Ballanti P, Sardella D, Chicca S, Manni M, Bonucci E, Taggi F (1996) Renal bone disease in 76 patients with varying degrees of predialysis chronic renal failure: a cross-sectional study. Nephrol Dial Transpl 11:813–819
Isakova T, Wahl P, Vargas GS, Gutierrez OM, Scialla J, Xie H, Appleby D, Nessel L, Bellovich K, Chen J et al (2011) Fibroblast growth factor 23 is elevated before parathyroid hormone and phosphate in chronic kidney disease. Kidney Int 79:1370–1378
Barreto FC, Barreto DV, FernandesCanziani ME, Tomiyama C, Higa A, Mozar A, Glorieux G, Vanholder R, Massy ZA, BarbosaDeCarvalho A (2014) Association between indoxyl sulfate and bone histomorphometry in pre-dialysis chronic kidney disease patients. J Braz Nefrol 36:289–296
Dhayat NA, Ackermann D, Pruijm M, Ponte B, Ehret G, Guessous I, Leichtle AB, Paccaud F, Mohaupt M, Fiedler GM et al (2016) Fibroblast growth factor 23 and markers of mineral metabolism in individuals with preserved renal function. Kidney Int 90:648–657
Lafage-Proust MH, Combe C, Barthe N, Aparicio M (1999) Bone mass and dynamic parathyroid function according to bone histology in nondialyzed uremic patients after long-term protein and phosphorus restriction. J Clin Endocrinol Metab 84:512–519
Graciolli FG, Neves KR, Barreto F, Barreto DV, Dos Reis LM, Canziani ME, Sabbagh Y, Carvalho AB, Jorgetti V, Elias RM, Schiavi S, Moysés RM (2017) The complexity of chronic kidney disease-mineral and bone disorder across stages of chronic kidney disease. Kidney Int. doi:10.1016/j.kint.2016.12.029
Drueke TB, Massy ZA (2016) Changing bone patterns with progression of chronic kidney disease. Kidney Int 89:289–302
Cosman F, Morgan DC, Nieves JW, Shen V, Luckey MM, Dempster DW, Lindsay R, Parisien M (1997) Resistance to bone resorbing effects of PTH in black women. J Bone Miner Res 12:958–966
Yan L, Schoenmakers I, Zhou B, Jarjou LM, Smith E, Nigdikar S, Goldberg GR, Prentice A (2009) Ethnic differences in parathyroid hormone secretion and mineral metabolism in response to oral phosphate administration. Bone 45:238–245
Fang Y, Ginsberg C, Seifert M, Agapova O, Sugatani T, Register TC, Freedman BI, Monier-Faugere MC, Malluche H, Hruska KA (2014) CKD-induced wingless/integration1 inhibitors and phosphorus cause the CKD-mineral and bone disorder. J Am Soc Nephrol 25:1760–1773
Sabbagh Y, Graciolli FG, O’Brien S, Tang W, dos Reis LM, Ryan S, Phillips L, Boulanger J, Song W, Bracken C et al (2012) Repression of osteocyte Wnt/beta-catenin signaling is an early event in the progression of renal osteodystrophy. J Bone Miner Res 27:1757–1772
Moe SM, Chen NX, Newman CL, Organ JM, Kneissel M, Kramer I, Gattone VH 2nd, Allen MR (2015) Anti-sclerostin antibody treatment in a rat model of progressive renal osteodystrophy. J Bone Miner Res 30:499–509
Bover J, Jara A, Trinidad P, Rodriguez M, Felsenfeld AJ (1999) Dynamics of skeletal resistance to parathyroid hormone in the rat: effect of renal failure and dietary phosphorus. Bone 25:279–285
Ferreira JC, Ferrari GO, Neves KR, Cavallari RT, Dominguez WV, Dos Reis LM, Graciolli FG, Oliveira EC, Liu S, Sabbagh Y et al (2013) Effects of dietary phosphate on adynamic bone disease in rats with chronic kidney disease—role of sclerostin? PLoS One 8:e79721
Nikolov IG, Joki N, Nguyen-Khoa T, Guerrera IC, Maizel J, Benchitrit J, Machado dos Reis L, Edelman A, Lacour B, Jorgetti V et al (2012) Lanthanum carbonate, like sevelamer-HCl, retards the progression of vascular calcification and atherosclerosis in uremic apolipoprotein E-deficient mice. Nephrol Dial Transpl 27:505–513
Tanaka H, Iwasaki Y, Yamato H, Mori Y, Komaba H, Watanabe H, Maruyama T, Fukagawa M (2013) p-Cresyl sulfate induces osteoblast dysfunction through activating JNK and p38 MAPK pathways. Bone 56:347–354
Nii-Kono T, Iwasaki Y, Uchida M, Fujieda A, Hosokawa A, Motojima M, Yamato H, Kurokawa K, Fukagawa M (2007) Indoxyl sulfate induces skeletal resistance to parathyroid hormone in cultured osteoblastic cells. Kidney Int 71:738–743
Mozar A, Louvet L, Godin C, Mentaverri R, Brazier M, Kamel S, Massy ZA (2012) Indoxyl sulphate inhibits osteoclast differentiation and function. Nephrol Dial Transpl 27:2176–2181
Iwasaki Y, Yamato H, Nii-Kono T, Fujieda A, Uchida M, Hosokawa A, Motojima M, Fukagawa M (2006) Administration of oral charcoal adsorbent (AST-120) suppresses low-turnover bone progression in uraemic rats. Nephrol Dial Transpl 21:2768–2774
Iwasaki Y, Kazama JJ, Yamato H, Shimoda H, Fukagawa M (2013) Accumulated uremic toxins attenuate bone mechanical properties in rats with chronic kidney disease. Bone 57:477–483
Hruska KA, Sugatani T, Agapova O, Fang Y (2017) The chronic kidney disease—mineral bone disorder (CKD-MBD): advances in pathophysiology. Bone. doi:10.1016/j.bone.2017.01.023
Metzinger-Le Meuth V, Burtey S, Maitrias P, Massy ZA, Metzinger L (2017) microRNAs in the pathophysiology of CKD-MBD: Biomarkers and innovative drugs. Biochim Biophys Acta 1863:337–345
Prisby R, Guignandon A, Vanden-Bossche A, Mac-Way F, Linossier MT, Thomas M, Laroche N, Malaval L, Langer M, Peter ZA et al (2011) Intermittent PTH(1–84) is osteoanabolic but not osteoangiogenic and relocates bone marrow blood vessels closer to bone-forming sites. J Bone Miner Res 26:2583–2596
Sun CY, Chang SC, Wu MS (2012) Suppression of Klotho expression by protein-bound uremic toxins is associated with increased DNA methyltransferase expression and DNA hypermethylation. Kidney Int 81:640–650
Towler DA (2011) Skeletal anabolism, PTH, and the bone-vascular axis. J Bone Miner Res 26:2579–2582
Yang K, Wang C, Nie L, Zhao X, Gu J, Guan X, Wang S, Xiao T, Xu X, He T et al (2015) Klotho protects against indoxyl sulphate-induced myocardial hypertrophy. J Am Soc Nephrol 26:2434–2446
Carvalho C, Alves CM, Frazao JM (2016) The role of bone biopsy for the diagnosis of renal osteodystrophy: a short overview and future perspectives. J Nephrol 29:617–626
Ketteler M, Elder GJ, Evenepoel P, Ix JH, Jamal SA, Lafage-Proust MH, Shroff R, Thadhani RI, Tonelli MA, Kasiske BL et al (2015) Revisiting KDIGO clinical practice guideline on chronic kidney disease-mineral and bone disorder: a commentary from a kidney disease: improving global outcomes controversies conference. Kidney Int 87:502–528
Gallieni M, De Luca N, Santoro D, Meneghel G, Formica M, Grandaliano G, Pizzarelli F, Cossu M, Segoloni G, Quintaliani G et al (2016) Management of CKD-MBD in non-dialysis patients under regular nephrology care: a prospective multicenter study. J Nephrol 29:71–78
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Rights and permissions
About this article
Cite this article
Massy, Z., Drueke, T. Adynamic bone disease is a predominant bone pattern in early stages of chronic kidney disease. J Nephrol 30, 629–634 (2017). https://doi.org/10.1007/s40620-017-0397-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-017-0397-7