Abstract
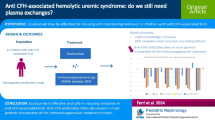
Atypical hemolytic uremic syndrome (aHUS) is a rare, chronic, life-threatening disease due to complement dysregulation. The use of early-onset plasma therapy is recommended, but optimal long-term treatment regimen is not well defined. Eculizumab, a monoclonal humanized anti-C5 antibody, has shown success in patients with aHUS. We report a 7-year-old girl with aHUS associated with factor H mutations successfully treated with eculizumab. Weekly plasma infusion (PI) of 25–30 ml/kg with short-term intensified PI during aHUS exacerbations was effective for 4.3 years. Progressive mild renal failure (stage 2) was attributed to chronic glomerular lesions. Subsequently, she exhibited aHUS exacerbation unresponsive to intensified PI. Eculizumab was initiated at 600 mg, resulting in immediate and complete inhibition of terminal complement activation. During the week following treatment, we observed a complete reversal of aHUS activity. She has been receiving 600 mg eculizumab every 2 weeks for the last 12 months. She had no aHUS exacerbation, and serum creatinine level returned to normal. In this patient, eculizumab led to control of PI-resistant aHUS exacerbation and chronic microangiopathic hemolytic activity. Clinical trials are ongoing to assess the safety and efficacy of this drug in the management of aHUS.


Similar content being viewed by others
References
Bresin E, Daina E, Noris M, Castelletti F, Stefanov R, Hill P, Goodship TH, Remuzzi G (2006) Outcome of renal transplantation in patients with non-Shiga toxin-associated hemolytic uremic syndrome: prognostic significance of genetic background. Clin J Am Soc Nephrol 1:88–99
Loirat C, Niaudet P (2003) The risk of recurrence of hemolytic uremic syndrome after renal transplantation in children. Pediatr Nephrol 18:1095–1101
Ariceta G, Besbas N, Johnson S, Karpman D, Landau D, Licht C, Loirat C, Pecoraro C, Taylor CM, Van de Kar N, Vandewalle J, Zimmerhackl LB (2009) Guideline for the investigation and initial therapy of diarrhea-negative hemolytic uremic syndrome. Pediatr Nephrol 24:687–696
Coppo P, Bussel A, Charrier S, Adrie C, Galicier L, Boulanger E, Veyradier A, Leblanc T, Alberti C, Azoulay E, Le Gall JR, Schlemmer B (2003) High-dose plasma infusion versus plasma exchange as early treatment of thrombotic thrombocytopenic purpura/hemolytic-uremic syndrome. Medicine (Baltimore) 82:27–38
Davin JC, Olie KH, Verlaak R, Horuz F, Florquin S, Weening JJ, Groothoff JW, Strain L, Goodship TH (2006) Complement factor H-associated atypical hemolytic uremic syndrome in monozygotic twins: concordant presentation, discordant response to treatment. Am J Kidney Dis 47:e27–30
Nathanson S, Ulinski T, Fremeaux-Bacchi V, Deschenes G (2006) Secondary failure of plasma therapy in factor H deficiency. Pediatr Nephrol 21:1769–1771
Warwicker P, Goodship TH, Donne RL, Pirson Y, Nicholls A, Ward RM, Turnpenny P, Goodship JA (1998) Genetic studies into inherited and sporadic hemolytic uremic syndrome. Kidney Int 53:836–844
Dragon-Durey MA, Fremeaux-Bacchi V (2005) Atypical haemolytic uraemic syndrome and mutations in complement regulator genes. Springer Semin Immunopathol 27:359–374
Hillmen P, Hall C, Marsh JC, Elebute M, Bombara MP, Petro BE, Cullen MJ, Richards SJ, Rollins SA, Mojcik CF, Rother RP (2004) Effect of eculizumab on hemolysis and transfusion requirements in patients with paroxysmal nocturnal hemoglobinuria. N Engl J Med 350:552–559
Chatelet V, Fremeaux-Bacchi V, Lobbedez T, Ficheux M, Hurault de Ligny B (2009) Safety and long-term efficacy of eculizumab in a renal transplant patient with recurrent atypical hemolytic-uremic syndrome. Am J Transplant 9:2644–2645
Davin JC, Gracchi V, Bouts A, Groothoff J, Strain L, Goodship T (2010) Maintenance of kidney function following treatment with eculizumab and discontinuation of plasma exchange after a third kidney transplant for atypical hemolytic uremic syndrome associated with a CFH mutation. Am J Kidney Dis 55:708–711
Gruppo RA, Rother RP (2009) Eculizumab for congenital atypical hemolytic-uremic syndrome. N Engl J Med 360:544–546
Larrea CF, Cofan F, Oppenheimer F, Campistol JM, Escolar G, Lozano M (2010) Efficacy of eculizumab in the treatment of recurrent atypical hemolytic-uremic syndrome after renal transplantation. Transplantation 89:903–904
Mache CJ, Acham-Roschitz B, Fremeaux-Bacchi V, Kirschfink M, Zipfel PF, Roedl S, Vester U, Ring E (2009) Complement inhibitor eculizumab in atypical hemolytic uremic syndrome. Clin J Am Soc Nephrol 4:1312–1316
Nurnberger J, Philipp T, Witzke O, Opazo Saez A, Vester U, Baba HA, Kribben A, Zimmerhackl LB, Janecke AR, Nagel M, Kirschfink M (2009) Eculizumab for atypical hemolytic-uremic syndrome. N Engl J Med 360:542–544
Rizvi MA, Vesely SK, George JN, Chandler L, Duvall D, Smith JW, Gilcher RO (2000) Complications of plasma exchange in 71 consecutive patients treated for clinically suspected thrombotic thrombocytopenic purpura-hemolytic-uremic syndrome. Transfusion 40:896–901
Olie KH, Florquin S, Groothoff JW, Verlaak R, Strain L, Goodship TH, Weening JJ, Davin JC (2004) Atypical relapse of hemolytic uremic syndrome after transplantation. Pediatr Nephrol 19:1173–1176
De S, Waters AM, Segal AO, Trautmann A, Harvey EA, Licht C (2010) Severe atypical HUS caused by CFH S1191L-case presentation and review of treatment options. Pediatr Nephrol 25:97–104
Richards A, Buddles MR, Donne RL, Kaplan BS, Kirk E, Venning MC, Tielemans CL, Goodship JA, Goodship TH (2001) Factor H mutations in hemolytic uremic syndrome cluster in exons 18-20, a domain important for host cell recognition. Am J Hum Genet 68:485–490
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lapeyraque, AL., Frémeaux-Bacchi, V. & Robitaille, P. Efficacy of eculizumab in a patient with factor-H-associated atypical hemolytic uremic syndrome. Pediatr Nephrol 26, 621–624 (2011). https://doi.org/10.1007/s00467-010-1719-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-010-1719-3