A 55-year-old man presented to the emergency department with 1 week of bilateral lower-extremity joint pain associated with painful skin nodules. He had a history of chronic recurrent alcoholic pancreatitis. He denied abdominal pain, nausea, or vomiting.
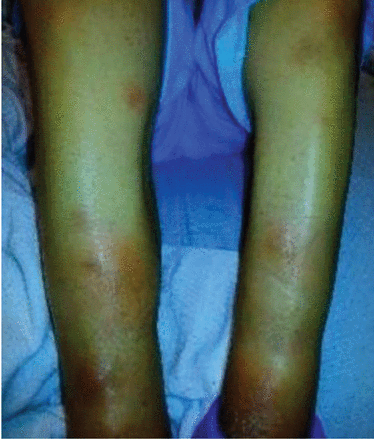
Physical examination revealed synovitis of the ankles and knees bilaterally and circumferential erythematous nodules 0.5 to 1.5 cm in diameter on the lower extremities (Figure 1).
The patient had multiple raised erythematous nodules on the lower extremities consistent with panniculitis.
Results of initial laboratory testing:
Alkaline phosphatase 300 IU/L (reference range 36–108)
Erythrocyte sedimentation rate 81 mm/h (0–15)
Lipase 20,000 U/L (16–61).
Skin biopsy of lower-extremity lesions showed lobular necrosis of the subcutaneous fat, consistent with pancreatic panniculitis (Figure 2). Computed tomography revealed an acute exacerbation of chronic (“acute-on-chronic”) pancreatitis, with pseudocyst formation and pancreatic duct dilation.
Biopsy study revealed pancreatic panniculitis. The subcutis showed mixed inflammation with characteristic “ghost adipocytes” of adipocyte necrosis (red box) (hematoxylin and eosin, × 10).
Because of the persistent elevation in the serum lipase level and the dilation of the pancreatic duct shown on imaging, endoscopic retro grade cholangiopancreatography was done to evaluate for malignant obstruction; it confirmed pancreatic duct stricture and dilation (Figure 3). Brush cytology study was negative for pancreatic or biliary malignancy. The pancreatic duct was dilated and stented, and the panniculitis and polyarthritis rapidly improved, with normalization of serum lipase levels. At a 3-month follow-up visit, the patient was asymptomatic with no recurrence of pancreatitis, panniculitis, or polyarthritis. He was subsequently lost to follow-up.
Endoscopic retrograde cholangiopancreatography confirmed pancreatic stricture (arrow) and dilation of the pancreatic duct (box).
AN ATYPICAL PRESENTATION OF A COMMON DISEASE
Epidemiology and pathophysiology
Pancreatitis, panniculitis, and polyarthritis syndrome is a rare systemic complication of pancreatic disease occurring most often in middle-aged men with an acute exacerbation of chronic pancreatitis and a history of alcohol use disorder.1,2 It is also associated with pancreatic pseudocyst, pancreas divisum, and pancreatic adenocarcinoma.3–6 It is characterized by systemic fat necrosis secondary to severe and persistent elevation of pancreatic enzymes. The mortality rate is high; in a case series of 25 patients, 24% died within days to weeks after admission.1
Clinical presentation and treatment
The diagnosis of pancreatitis, panniculitis, and polyarthritis syndrome is often missed. Abdominal pain is mild or absent in over 60% of patients.1 Therefore, a high index of suspicion is required for early diagnosis.
The differential diagnosis includes sarcoidosis (including Löfgren syndrome), subcutaneous infection, and vasculitis. “Ghost adipocytes” on skin biopsy are pathognomonic for pancreatic panniculitis and are the result of saponification; they appear to be anuclear, with basophilic material throughout the cytoplasm.7 Arthrocentesis of affected joints may reveal thick, creamy material, rich in triglycerides, which is diagnostic of pancreatic arthritis.1,8
Treatment relies on correction of the underlying pancreatic pathology. Pancreatitis, panniculitis, and polyarthritis syndrome has been successfully treated by cyst gastrostomy, pancreatic duct stenting, and pancreaticoduodenectomy.7,9–11
TAKE-HOME POINTS
Pancreatitis, panniculitis, and polyarthritis syndrome mimics rheumatologic disease and often presents without abdominal pain.
The diagnosis is confirmed by the presence of elevated serum lipase or amylase, pancreatic imaging showing pancreatitis, and ghost adipocytes on skin biopsy.
Treatment is aimed at correcting the underlying pancreatic abnormality.
- Copyright © 2018 The Cleveland Clinic Foundation. All Rights Reserved.